MEDICARE CCM

MEDICARE CCM IN LESS THAN A MINUTE
WHAT IS THE MEDICARE CCM PROGRAM (M-CCM)

When it comes to Medicare, reimbursement has always been the problem. Everyone knows it. To address this, CMS created the Medicare Chronic Care Management Program (M-CCM), which very few clinics/organizations are fully participating, which is an equitable reimbursement and exceptional patient care, utilization, and care management opportunity.
The program covers medically necessary care management activities that are performed outside of a face-to-face in-person visit by clinical staff on behalf of Medicare patients with complex health care needs.
- Creates checklists and protocols to manage chronic diseases for eligible Medicare patients via mid-level nurse telehealth visits, which after an initiating visit, are not required to be in person or face-to-face.
- Mid-level nurses (who assign their billing rights to the clinic or organization and work under their NPI and insurance), work under the direction of a physician and conduct proactive monthly telehealth outreach.
- Specific care plans for each patient are agreed upon between the care manager (NP), patient, and physician.
- Includes five sets of reimbursement codes which are reported monthly on a timed basis, each set with a base code of 20-to-60-minutes and an add-on code for each additional 30 minutes.
- CMS has configured the program to help clinics/organizations deliver exceptional patient care, increase reimbursement, and improve patient relationships.
- CMS calculated the program reduces annual per patient Total Cost of Care $888.00 by reducing ER and Urgent Care visits and hospital admissions.
Participating in the M-CCM Program will helps your clinic/organization and providers reimagine what it means to care for Medicare patients with chronic disease. Because it takes care management and makes it proactive and relational, rather than reactive and transactional.
M-CCM IS DIFFERENT FROM YOUR CURRENT CCM & TELEHEALTH OUTREACH ACTIVITIES
M-CCM does not change or take away from your current CCM & telehealth outreach activities – It adds to them.
The Difference:
- Patients must have 2 or more chronic conditions to be eligible.
- Patients must explicitly ‘opt-in’ to the program.
- Specific care management templates and engagement policies are required to make it billable.
- Each patient receives at least 20 minutes of telehealth interaction per month.
- Each interaction is billed at MAC location reimbursement level.
- Billing is under the general CPT Code 99490.
- Additional billings are available depending on the level of interaction under the CPT Codes: 99424, 99425, 99426, 99437, 99439, 99487, 99489, and 99491.
M-CCM LANDSCAPE
The Opportunity
- Significant Financial Incentive. The per-eligible-patient per-month reimbursement on patients you are already serving that can be captured with the program can make a huge difference to your clinics/organization and providers,
- Improved Patient Care. Positive outcome results that improve patient relationships.
The Challenges
- Compliance. Procedures must be followed to make M-CCM CPT codes billable.
- Implications On Operations. Additional staffing and workload are required if handled internally.
- Patient Engagement. Specific policies must be followed.
- Program Level Implementation. Initial clinic and physician level education, clinical policy, patient identification, and more are required.
- Staffing. Staffing levels continue to be challenged, depleted, and costly.
- Patient Onboarding. Properly identifying patients and an effective outreach strategy is required.
- Poor Vendor Performance. Most CCM vendors utilize a flawed business model and fail to successfully onboard a sufficient number of eligible patients.
- ACO Failure. ACO’s should handle M-CCM. However, most cannot because they lack the funding, technology, and staff to properly manage the program.
Eligible Patient’s Enrollment
Not all eligible Medicare patient will opt-in the program, but those that do value having a nurse, NP, or a PA that they can talk to every month. They also appreciate the:
- Dedicated personal care managers.
- Comprehensive care plans.
- Reduced annual and out-of-pocket medical expenses.
- Health goal setting.
- Medication management and support.
- 24/7 support.
Participation is Complex
It can be a Large-Scale Project
- Your clinic/organization and providers must overcome complex issues across multiple clinics and/or doctors.
- Must align with the goals of your clinic/organization and physicians, which are related – but different.
- Requires the implementation of strategies that are tied to your clinic/organization’s culture and relationship with ownership/board.
- Your clinic/organization or professional service provider must fully “staff up” for implementation.
- The effort must help your clinic/organization gain a unique advantage in overcoming the biggest obstacle to success – patient recruitment and onboarding.
- Must utilize SaaS or AI technology for program management.
The illustration below shows the many steps that must be achieved before your clinic or organization and provides can begin onboarding eligible patients.
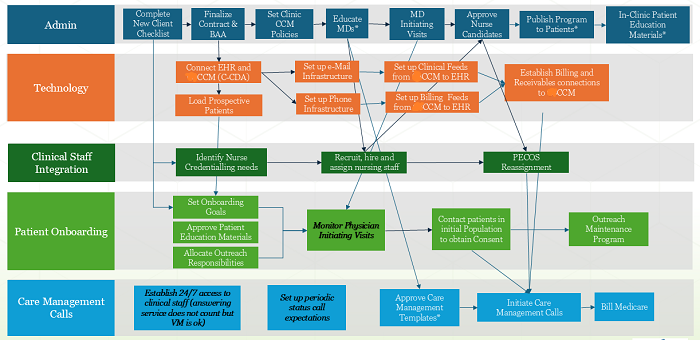
In addition, CMS requires patient engagement policies be strictly followed for the program CPT codes to be billable. This is where many ACO’s, vendor’s, clinics, organizations, and providers – have had problems, gotten frustrated, and have given up on the program.
APPROACHING M-CCM

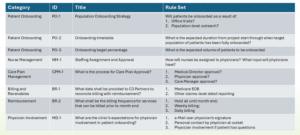
Successfully participating in the program requires overcoming several challenges and obstacles. The first step starts with answering a few very important questions:
- Do you know for sure that your clinic/organization and providers are currently participating in the M-CCM Program?
- Have you ever had an M-CCM Feasibility Analysis done?
- Who is doing or will be doing the heavy lifting in your M-CCM efforts – Your clinic/organization or a professional service provider (vendor)?
A Feasibility Analysis is Required for Success
Without a deep analysis, program success is nearly impossible. This is why both vendors and ACOs have failed to generate adequate program adoption and enrollments. The program is a complex initiative. It is very much like a new business venture. Therefore, it is prudent and desirable to first test assumptions, define strategies, evaluate data, and develop plans that would enable results that meet the goals and needs of your clinic, organization, and providers. You cannot just jump into it. Accordingly, a Feasibility Analysis is required.
The analysis completes all preliminary work necessary for program success (i.e. establishing clinical policy, providing physician education, conducting patient identification, developing the patient engagement/onboarding strategy, and more). This combined with a full-service support system, SaaS technology, and a team experienced in big initiatives – your clinic, organization, and providers can double or even triple average cadence results.
OUR OFFERING
Our offering is built to help your clinic/organization and providers with evaluating, implementing, and operating this Medicare-specific CCM program. Here are our key success offerings:
- M-CCM Feasibility Analysis – Should you have the program? What are the metrics, physician profiles, and cultures that will support success? What physicians and patients should be incorporated? Who will hire / contract for mid-level billers? At what fee (if any) will the physicians be charged for mid-level services?
- M-CCM Implementation – We develop and roll out policies supporting the program. Implementation services also include education of administrative and clinical staff, developing patient education materials, setting up organizational responsibilities for patient onboarding, etc.).
- Software Operations – Unique software manages the scheduling, clinical documentation, telehealth / calling, and executive dashboarding. It integrates with your clinic/organization’s EHR and billing system.
- Clinical Staffing – Our flexible staffing model supports a range of clinic-level strategies. At the full concierge level, we hire, train, and manage all mid-level staff (usually Nurse Practitioners). This model can be either a permanent arrangement, or part of your startup-strategy where we phase out our team as you roll in your own employees.
WHY OUR SERVICE PROVIDER’S PLATFORM IS YOUR BEST CHOICE
Many healthcare executives are curious about the program because they are doing CCM and telehealth outreach activities. Many claim their ACO handles the program, which have been unsuccessful, or have contracted with a CCM vendor on a fully-outsourced contract (staffing and all other services), which had an initial set of enthusiasm with eligible patients and physicians but has fallen off.
Fall off is most often due to not having set a proper level of expectations among physician staff and not having any performance metrics beyond basic billing data. These include:
- No indication of how many patients are currently enrolled;
- No indication of what percentage of eligible patients are enrolled;
- No software tools that report on staff efficiency; and
- No easy access to reporting on CPT 99490 and 99487 billing.
These Issues Are is Why Top-Performing Clinics/Organizations Should Only Utilize the Services of Top-Performing Professionals for M-CCM.
- Our service provider partner is the most qualified and the ‘best-in-class’ at identifying M-CCM feasibility and conducting program management.
- Their skill-set, strategies, tools, and support provide the structure that ensures success.
- Their team is deeply experienced in healthcare and large-scale program implementation and operations.
- Their comprehensive understanding of regulatory requirements and advanced proprietary SaaS technology and continuous updates in response to industry changes, make their platform crucial for meeting quality metrics and achieving better patient outcomes.
This makes them ideal for conducting the Feasibility Analysis and becoming your program management service partner.
The M-CCM Program is a major initiative for every clinic/organization and their providers that goes down the path. In many ways it is a lot like a new business venture. Your best chance of success is to first find out if it is feasible to fully participate – and align with a team that provides the best technology and is experienced in big initiatives.
CMS M-CCM PROGRAM DATA SET SNAPHOT
 We will email you a CMS M-CCM Program Data Set Snapshot that shows your total number of providers, Medicare beneficiaries, eligible beneficiaries, billing of the program’s primary CPT code, your state average MAC reimbursement, and the additional reimbursement and Total Cost of Care savings with 20% – and 30% – eligible patient enrollment – that your clinic/organization and providers can capture from the program on eligible patients you are already serving. It will break down the numbers in quite simple language.
We will email you a CMS M-CCM Program Data Set Snapshot that shows your total number of providers, Medicare beneficiaries, eligible beneficiaries, billing of the program’s primary CPT code, your state average MAC reimbursement, and the additional reimbursement and Total Cost of Care savings with 20% – and 30% – eligible patient enrollment – that your clinic/organization and providers can capture from the program on eligible patients you are already serving. It will break down the numbers in quite simple language.
Click Here or see the link below to request your clinic/organization’s CMS Data Snapshot.
SUPPORTING MATERIALS
Take a few moments to download our info and CMS data supporting materials below.
- Live Well A.P.S. CMS Fee Increase and Timely Solution Flyer (pdf).
- Live Well A.P.S. Medicare CCM Program Brochure (pdf).
- Frequently Asked Questions (pdf).
- CMS MLN M-CCM Brochure (pdf).
- CMS C2C M-CCM Patient Brochure (pdf).
- Medicare Chronic Care Management for Seniors (link).
- CMS Outreach and Education on CCM report (pdf).
- Mathematica 2017 report on CCM (pdf). (This is an important study, but a bit long. See page 64 for the Bottom Line).
- 2025 National Health Expenditure Projections 2024-2033 (pdf),
